Doctor saving lives in Africa was inspired by colleagues who saved his son - and wants help to save even more children

A doctor whose new-born baby was saved by the NHS is saving other children’s lives in Africa – and says he could help even more for the price of a cup of coffee.
Mikey Bryant, who works for the acute clinical team and out-of-hours service in Swansea, has spent years working in Liberia where he helped set-up a vital malnutrition programme which has already saved the lives of thousands of babies and young children.
The project at the ELWA Hospital in the country’s capital Monrovia was helped on its way with funding by the former ABMU Health Board, Swansea Bay UHB’s predecessor. Now the current Swansea Bay Health Charity continues to provide support.
And, despite weathering the challenges of Covid-19, the project has continued to expand, providing vital health provision to some of the poorest people in Africa, who would otherwise not be able to receive healthcare – and who would be facing certain death.
Dr Bryant spent nine years in Africa as a child in Senegal which triggered his desire to study medicine so he could return to the continent to help. He volunteers at the hospital with wife Dr Bethany Bryant - who is a paediatric doctor - at Singleton Hospital when working in Wales.
And after helping save the lives of hundreds of children in Africa, the couple needed some medical support of their own, when Bethany gave birth to the couple’s first child. Mikey was away working in Liberia in November 2021 when Bethany, who was back home in Swansea, went into labour 11 weeks early, prompting a frantic dash by her husband to get home. Their son Finley eventually spent seven weeks in Singleton Hospital’s Neonatal Intensive Care Unit (NICU).
Dr Bryant said: “I didn’t know if Finley was going to make it. I was expecting to land at Heathrow to get a phone call telling me I needed to call Singleton.
“But the care he received there was incredible, so far away and above what we are doing in Liberia, and it really inspired us.
“All we have there is a six-bed new-born space and we’re only able to do basic things like feeding and giving oxygen. We have one working incubator. It’s not a real NICU, but at least we have something and we do our best. The staff out there work extremely hard with extremely limited resources.
“Three of us went back out to Liberia in June last year for eight months, with a focus to expand the new-born care space, and a lot of that came from Finley’s experience, which we wanted to reproduce.”

A mother and child who were helped by staff at Elwa Hospital
The project at ELWA Hospital began with just 12 beds on a single ward, and a clinic for under-fives to provide basic treatment. The country’s Ministry of Health contacted them requesting they start a malnutrition programme, and the hospital soon increased to having 30 beds.
Then Covid struck.
“Covid destroyed the economy and meant there was no way to get food into the country,” said Dr Bryant.
“There were malnourished children everywhere. That meant between March and July that year we doubled in size again, and we had to expand the under-fives clinic from three days to five. We started doing an out-patient feeding programme and things got progressively busier. We now had 20 beds in our emergency department, a total of 55, and we were always full.”
The life-saving service is supported by local staff who are trained under an Emergency Triage Assessment and Treatment (ETAT) programme, which prepares them to work in resource-limited settings, and teaches them how to care for a sick child within the first 24 hours of arrival.
“The outcomes are better, and it has led to loads of lives being saved,” said Mikey.
“We are currently running at a high capacity of between 300 and 400 admissions every month, about ten times the figure from five years ago.
“We are the biggest malnutrition programme within Liberia, and if you took it away there would be thousands of children who would have nowhere to go when they are sick. It is big. It has turned out much bigger than anyone anticipated.
“The role of Swansea Bay Health Charity was key in starting the process five years ago, by continuing to support staff. We now have eight staff members at the hospital who the charity’s supports, as well as between 20 and 30% of the medication supplies.
“It is a lifeline because the poverty in Liberia is on another level. You will meet children who are starving, or who have undiagnosed tuberculosis or HIV.
“Through this programme you get the diagnosis, you start the treatment, and they get better, where otherwise they would certainly die. Survival rates on nutrition in-feeding programmes are 95% which is wonderful.”
He added: “I love working in Swansea and what we do for patients here. I think we’ve got a good health board, and the NHS is the best organisation in the world.
“But we have an opportunity to do something for a group of people who do not have an NHS, who don’t have free medicine at the point of care.
“We have put in a system where children within an hour of arriving can have all those life-saving first medicines, with no delays.”
However, despite support from the Swansea Bay Health Charity and other charities, funding remains a challenge.
“One-off donations are kind and welcome, but regular donating helps us budget from one day to the next; we are able to plan and to strategize. It is a huge help.
“I would love to see more people signed up to help us out.
“For example, if someone wants to support a child with severe malnutrition through the in-patient feeding unit, that is about £60 for a week, and that is all it takes to save a child’s life.
“The cost of supporting a child visiting the outpatient feeding programme would be even cheaper.
“If we had 300 people signed up to give £10 a month that would make £3,000 which would make a massive difference – it would cover the whole of the outpatient service completely.
“A coffee on the high street costs around £5, so it’s just the price of two cups of coffee a month.
“I am signed up and donate. I don’t take any personal money, I pay my own air fare, I volunteer my own time. All donated money goes straight to the children. I would encourage as many people as possible to donate because we need the help.
He added: “It is the most transformative thing I have ever done. Every day, whatever I am doing, if it is a ward round and starting a treatment, or doing some training with some staff, you know the day is going to have an impact and move things forward for some sick children and I think that is beautiful.
“These children would be dead if we didn’t do this. The work is life-changing, and these children are worth it.”
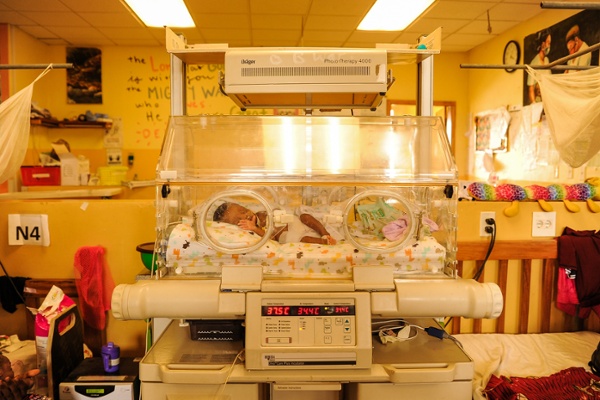
A baby in the incubator at Elwa Hospital
MIRACLE
The three-year-old was brought to ELWA hospital from deep inside the African bush. She had a haemoglobin level of 3 – she should have been between 12 and 14. She was breathing approximately 80 – 90 breaths a minute, instead of 20 – 30.
Dr Bryant said: “She was in a coma, I thought there is no way she is going to make it. I thought this isn’t going to be a miracle at all. But we set up some blood, antibiotics, antimalarials, got oxygen going.
“I went to bed that night thinking this is too far, there is no way this child is going to survive.
“Then I came in next day and Miracle is there sitting up, off the oxygen, having received the blood within 30 minutes of her arrival in hospital. Her breaths were down to 40, and was eating some rice and fish.
“The turnaround in 24 hours was down to the ETAT training. Staff knew they had a sick child and these are the things that are wrong, and knew exactly what to do, what medicines to use, exactly the doses. They saved Miracle’s life.”
LUCKY BOY
Another child from deep in the bush who arrived with malnutrition called Kwashioraor, which meant he had swollen extremities, his hands and a pot belly. He was completely flat and unresponsive. He had had no food for over a week. His mother was dead, his father had disappeared and was being cared for by an aunt with learning difficulties.
“The staff just clicked into action,” said Dr Bryant.
“Within seconds they’d got a nasal-gastric tube fitted, oxygen, some simple interventions, and over that week his swelling went down.
“By day three or four we took out the tube and Lucky Boy was fending for himself. He was on a thick therapeutic milk, and he just got bigger and bigger and bigger.
“By the time he left he was doing laps of the ward, running about, playing with the toys. Seeing that transformation was incredible”.
You can help the malnutrition and paediatric project at Elwa Hospital via Africa Health Links, which is one of hundreds of individual funds that come under the umbrella of Swansea Bay Health Charity.
This is the health board’s official charity. Money raised is used for equipment, staff training, research and special projects for the benefit of our patients and staff, above and beyond what the NHS can provide.
It can be found by visiting https://swanseabayhealthcharity.enthuse.com/donate and selecting Africa Health Links.
If this story has inspired you to raise funds for your local NHS then Swansea Bay Health Charity would love to hear from you.
Email the charity team at: swanseabay.healthcharity@wales.nhs.uk.
Swansea Bay Health Charity (registered charity number 1122805) is the official charity of Swansea Bay University Health Board.
Rydym yn croesawu gohebiaeth a galwadau ffôn yn y Gymraeg neu'r Saesneg. Atebir gohebiaeth Gymraeg yn y Gymraeg, ac ni fydd hyn yn arwain at oedi. Mae’r dudalen hon ar gael yn Gymraeg drwy bwyso’r botwm ar y dde ar frig y dudalen.
We welcome correspondence and telephone calls in Welsh or English. Welsh language correspondence will be replied to in Welsh, and this will not lead to a delay. This page is available in Welsh by clicking ‘Cymraeg’ at the top right of this page.